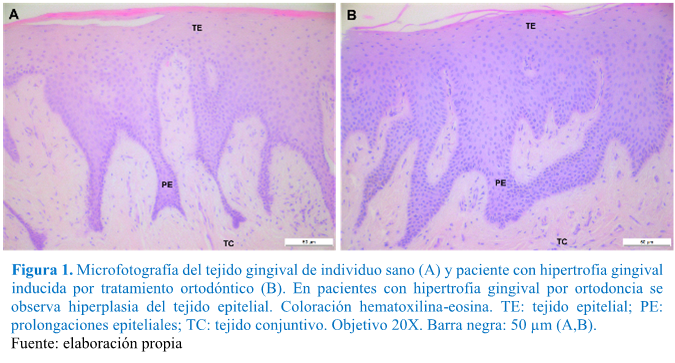
Immunolocalización de s100a4 y α-sma en tejidos gingivales de pacientes con hipertrofia gingival por tratamiento ortodóntico: estudio preliminar
Immunolocalización de s100a4 y α-sma en tejidos gingivales de pacientes con hipertrofia gingival por tratamiento ortodóntico: estudio preliminar Immunolocalization of s100a4 and α-sma in gingival tissues of patients with gingival hypertrophy due to orthodontic treatment: preliminary study
How to Cite
Download Citation

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Show authors biography
Most read articles by the same author(s)
- Jonathan Harris Ricardo, Leidy Álvarez Ricardo, Antonio Díaz Caballero, Diagnostic parameters of cleidocranial dysplasia: a low frequent disease , Archivos de Medicina (Manizales): Vol. 17 No. 2
Objective: The present work seeks to determine the presence and distribution of markers of the epithelial-mesenchymal transition (EMT) (S-100A4 and alpha-smooth muscle actin-α-SMA) in gingival tissues of patients affected by Gingival overgrowth (GO) due to orthodontics. GO is an exaggerated increase in gingival tissue whose pathogenesis is unknown. However, it has been reported that the epithelial-mesenchymal transition as a process involved in other types of GO. Materials and methods: Descriptive study that included the analysis of gingival tissues of healthy individuals (n = 6) and patients with GO due to orthodontic treatment (n = 6). The identification and location of S-100A4 and α-SMA was performed by immunohistochemistry, determining the cell types involved in each expression. Results: In healthy individuals, a S100A4 label was observed in Langerhans cells and α-SMA, in the vascular endothelium of all samples analysed. However, in patients with GO due to orthodontics, intense staining of S100A4 was recorded in gingival fibroblasts, Langerhans cells, vascular endothelium, and areas adjacent to blood vessel rupture while α-SMA expression was present in the endothelium vascular and gingival fibroblasts. Conclusion: Differential immunomarking of EMT markers in gingival tissues of patients with gingival overgrowth due to orthodontics suggests the role of EMT in the pathogenesis of this pathology
Article visits 880 | PDF visits 46
Downloads
- Gameiro GH, Magalhães IB, Szymanski MM, Andrade AS. Is the main goal of mastication achieved after orthodontic treatment? A prospective longitudinal study. Dental Press J Orthod. 2017; 22:72–8. DOI: 10.1590/2177-6709.22.3.072-078.oar
- Seixas MR, Costa-Pinto RA, Martins T. Gingival esthetics: an orthodontic and periodontal approach. Dental Press J. Orthod. 2012; 17:190–201. DOI: 10.1590/S2176-94512012000500025
- Perkowski K, Baltaza W, Conn DB, Marczyńska-Stolarek M, Chomicz L. Examination of oral biofilm microbiota in patients using fixed orthodontic appliances in order to prevent risk factors for health complications. Ann Agric Environ Med. 2019; 26(2):231–5. DOI: 10.26444/aaem/105797
- Reichert C, Kutschera E, Plötz C, Scharf S, Gölz L, Fimmers R, et al. Incidence and severity of gingival invaginations associated with early versus late initiation of orthodontic space closure after tooth extraction: A multicenter pilot and randomized controlled trial. J Orofac Orthop. 2017; 78(5):415–25. DOI: 10.1007/s00056-017-0098-9
- Pinto AS, Alves LS, Zenkner JE do A, Zanatta FB, Maltz M. Gingival enlargement in orthodontic patients: Effect of treatment duration. Am J Orthod Dentofacial Orthop. 2017; 152(4):477–82. DOI: 10.1016/j.ajodo.2016.10.042
- Drăghici EC, CrăiŢoiu Ş, MercuŢ V, Scrieciu M, Popescu SM, Diaconu OA, et al. Local cause of gingival overgrowth. Clinical and histological study. Rom J Morphol Embryol. 2016; 57(2):427–35
- Rodríguez Vásquez A, Fernández García L, Valladares Trochez E. Prevalencia de agrandamiento y retracción gingival en pacientes con tratamiento de ortodoncia. PC. 2018; 13:21-31. https://doi.org/10.5377/pc.v13i0.5918
- Manzur-Villalobos I, Díaz-Rengifo IA, Manzur-Villalobos D, Díaz-Caballero AJ. Agrandamiento gingival farmacoinducido: Serie de casos. Univ. Salud. 2018; 20(1):89-96. https://dx.doi.org/10.22267/rus.182001.113
- Rahul M, Gauba K, Gorwade N, Kumar A. Rare case report of idiopathic gingival fibromatosis in childhood and its management. BMJ Case Rep. 2019; 12(1):e227942. DOI: 10.1136/bcr-2018-227942
- Zanatta FB, Ardenghi TM, Antoniazzi RP, Pinto TMP, Rösing CK. Association between gingivitis and anterior gingival enlargement in subjects undergoing fixed orthodontic treatment. Dental Press J Orthod. 2014; 19(3):59–66. DOI: 10.1590/2176-9451.19.3.059-066.oar
- Gursoy UK, Sokucu O, Uitto V-J, Aydin A, Demirer S, Toker H, et al. The role of nickel accumulation and epithelial cell proliferation in orthodontic treatment-induced gingival overgrowth. Eur J Orthod. 2007; 29(6):555–8. DOI: 10.1093/ejo/cjm074
- Şurlin P, Rauten AM, Pirici D, Oprea B, Mogoantă L, Camen A. Collagen IV and MMP-9 expression in hypertrophic gingiva during orthodontic treatment. Rom J Morphol Embryol. 2012; 53(1):161–5
- Niţulescu EA, Crăiţoiu MM, Baniţă MI, Drăghici E, Crăiţoiu Ş. The involvement of TGF-β1 and CTGF in regional gingival overgrowth. Rom J Morphol Embryol. 2012; 53(1):143–50
- Gonzalez DM, Medici D. Signaling mechanisms of the epithelial-mesenchymal transition. Sci Signal. 2014; 7(344):re8–re8. DOI: 10.1126/scisignal.2005189
- Lamouille S, Xu J, Derynck R. Molecular mechanisms of epithelial–mesenchymal transition. Nat Rev Mol Cell Biol. 2014; 15(3):178–96. DOI: 10.1038/nrm3758
- Sume SS, Kantarci A, Lee A, Hasturk H, Trackman PC. Epithelial to Mesenchymal Transition in Gingival Overgrowth. Am J Pathol. 2010; 177(1):208–18. DOI: 10.2353/ajpath.2010.090952
- Fu MM, Chin Y-T, Fu E, Chiu H-C, Wang L-Y, Chiang C-Y, et al. Role of Transforming Growth Factor-beta1 in Cyclosporine-Induced Epithelial-to-Mesenchymal Transition in Gingival Epithelium. J Periodontol. 2015; 86(1):120–8. DOI: 10.1902/jop.2014.130285
- Carlson RV, Boyd KM, Webb DJ. The revision of the Declaration of Helsinki: past, present and future. Br J Clin Pharmacol. 2004; 57(6):695–713. DOI: 10.1111/j.1365-2125.2004.02103.x
- Arora H, Madapusi BT, Ramamurti A, Narasimhan M, Periasamy S, Rao SR. Immunohistochemical Localization of Epithelial Mesenchymal Transition Markers in Cyclosporine A Induced Gingival Overgrowth. J Clin Diagn Res. 2016; 10(8):ZC48-52. DOI: 10.7860/JCDR/2016/20808.8271
- Nan L, Zheng Y, Liao N, Li S, Wang Y, Chen Z, et al. Mechanical force promotes the proliferation and extracellular matrix synthesis of human gingival fibroblasts cultured on 3D PLGA scaffolds via TGF‑β expression. Mol Med Rep. 2019; 19(3):2107-2114. DOI: 10.3892/mmr.2019.9882
- Pascu EI, Pisoschi CG, Andrei AM, Munteanu MC, Rauten AM, Scrieciu M, et al. Heterogeneity of collagen secreting cells in gingival fibrosis--an immunohistochemical assessment and a review of the literature. Rom J Morphol Embryol. 2015; 56(1):49–61
- Simancas-Escorcia V, Díaz-Caballero A. Fisiología y usos terapéuticos de los fibroblastos gingivales. Odous Científica. 2019; 20(1): 41-57
- Bresnick AR. S100 proteins as therapeutic targets. Biophys Rev. 2018; 10(6):1617–29. DOI: 10.1007/s12551-018-0471-y
- Strutz F, Okada H, Lo CW, Danoff T, Carone RL, Tomaszewski JE, et al. Identification and characterization of a fibroblast marker: FSP1. J Cell Biol. 1995; 130(2):393–405. DOI:10.1083/jcb.130.2.393
- Okada H, Danoff TM, Kalluri R, Neilson EG. Early role of Fsp1 in epithelial-mesenchymal transformation. Am J Physiol. 1997; 273(4):F563-74. DOI: 10.1152/ajprenal.1997.273.4.F563
- Xie Y, Liao J, Yu Y, Guo Q, Yang Y, Ge J, et al. Endothelial‑to‑mesenchymal transition in human idiopathic dilated cardiomyopathy. Mol Med Rep. 2018; 17(1):961-969. DOI: 10.3892/mmr.2017.8013
- Nishitani Y, Iwano M, Yamaguchi Y, Harada K, Nakatani K, Akai Y, et al. Fibroblast-specific protein 1 is a specific prognostic marker for renal survival in patients with IgAN. Kidney Int. 2005; 68(3):1078-85. DOI: 10.1111/j.1523-1755.2005.00500.x
- Piera-Velazquez S, Jimenez SA. Endothelial to Mesenchymal Transition: Role in Physiology and in the Pathogenesis of Human Diseases. Physiol Rev. 2019; 99(2):1281-1324. DOI: 10.1152/physrev.00021.2018
- Moccia F, Negri S, Shekha M, Faris P, Guerra G. Endothelial Ca2+ Signaling, Angiogenesis and Vasculogenesis: just What It Takes to Make a Blood Vessel. Int J Mol Sci. 2019; 20(16). pii: E3962. DOI: 10.3390/ijms20163962
- Stempien-Otero A, Kim D-H, Davis J. Molecular networks underlying myofibroblast fate and fibrosis. J Mol Cell Cardiol. 2016; 97:153–61. DOI: 10.1016/j.yjmcc.2016.05.002
- Yuan Q, Tan RJ, Liu Y. Myofibroblast in Kidney Fibrosis: Origin, Activation, and Regulation. Adv Exp Med Biol. 2019; 1165:253-283. DOI: 10.1007/978-981-13-8871-2_12